Telemedicine Appointments Are Now Available
Your Trusted Double - Board Certified Gastroenterologist





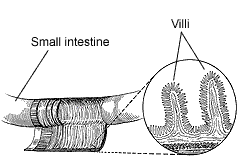
Celiac disease is a digestive disease that damages the small intestine and interferes with absorption of nutrients from food. People who have celiac disease cannot tolerate a protein called gluten, which is found in wheat, rye, barley, and possibly oats. When people with celiac disease eat foods containing gluten, their immune system responds by damaging the small intestine. Specifically, tiny fingerlike protrusions, called villi, on the lining of the small intestine are lost. Nutrients from food are absorbed into the bloodstream through these villi. Without villi, a person becomes malnourished–regardless of the quantity of food eaten.Because the body’s own immune system causes the damage, celiac disease is considered an autoimmune disorder. However, it is also classified as a disease of malabsorption because nutrients are not absorbed. Celiac disease is also known as celiac sprue, nontropical sprue, and gluten-sensitive enteropathy.
Amaranth
Villi on the lining of the small intestine help absorb nutrients.
Celiac disease affects people differently. Some people develop symptoms as children, others as adults. One factor thought to play a role in when and how celiac appears is whether and how long a person was breastfed–the longer one was breastfed, the later symptoms of celiac disease appear and the more atypical the symptoms. Other factors include the age at which one began eating foods containing gluten and how much gluten is eaten.
Symptoms may or may not occur in the digestive system. For example, one person might have diarrhea and abdominal pain, while another person has irritability or depression. In fact, irritability is one of the most common symptoms in children.
Symptoms of celiac disease may include one or more of the following:
Anemia, delayed growth, and weight loss are signs of malnutrition–not getting enough nutrients. Malnutrition is a serious problem for anyone, but particularly for children because they need adequate nutrition to develop properly.
Some people with celiac disease may not have symptoms. The undamaged part of their small intestine is able to absorb enough nutrients to prevent symptoms. However, people without symptoms are still at risk for the complications of celiac disease.
Diagnosing celiac disease can be difficult because some of its symptoms are similar to those of other diseases, including irritable bowel syndrome, Crohn’s disease, ulcerative colitis, diverticulosis, intestinal infections, chronic fatigue syndrome, and depression.
Recently, researchers discovered that people with celiac disease have higher than normal levels of certain antibodies in their blood. Antibodies are produced by the immune system in response to substances that the body perceives to be threatening. To diagnose celiac disease, physicians test blood to measure levels of antibodies to endomysium and tissue transglutaminase.
If the tests and symptoms suggest celiac disease, the physician may remove a tiny piece of tissue from the small intestine to check for damage to the villi. This is done in a procedure called a biopsy: the physician eases a long, thin tube called an endoscope through the mouth and stomach into the small intestine, and then takes a sample of tissue using instruments passed through the endoscope. Biopsy of the small intestine is the best way to diagnose celiac disease.
Screening for celiac disease involves testing asymptomatic people for the antibodies (see above). Americans are not routinely screened for celiac disease. However, because celiac disease is hereditary, family members–particularly first-degree relatives–of people who have been diagnosed may need to be tested for the disease. About 10 percent of an affected person’s first-degree relatives (parents, siblings, or children) will also have the disease. The longer a person goes undiagnosed and untreated, the greater the chance of developing malnutrition and other complications.
The only treatment for celiac disease is to follow a gluten-free diet–that is, to avoid all foods that contain gluten. For most people, following this diet will stop symptoms, heal existing intestinal damage, and prevent further damage. Improvements begin within days of starting the diet, and the small intestine is usually completely healed–meaning the villi are intact and working–in 3 to 6 months. (It may take up to 2 years for older adults.)
The gluten-free diet is a lifetime requirement. Eating any gluten, no matter how small an amount, can damage the intestine. This is true for anyone with the disease, including people who do not have noticeable symptoms. Depending on a person’s age at diagnosis, some problems, such as delayed growth and tooth discoloration, may not improve.
A small percentage of people with celiac disease do not improve on the gluten-free diet. These people often have severely damaged intestines that cannot heal even after they eliminate gluten from their diet. Because their intestines are not absorbing enough nutrients, they may need to receive intravenous nutrition supplements. Drug treatments are being evaluated for unresponsive celiac disease. These patients may need to be evaluated for complications of the disease.
A gluten-free diet means avoiding all foods that contain wheat (including spelt, triticale, and kamut), rye, barley, and possibly oats–in other words, most grain, pasta, cereal, and many processed foods. Despite these restrictions, people with celiac disease can eat a well-balanced diet with a variety of foods, including bread and pasta. For example, instead of wheat flour, people can use potato, rice, soy, or bean flour. Or, they can buy gluten-free bread, pasta, and other products from special food companies.
Whether people with celiac disease should avoid oats is controversial because some people have been able to eat oats without having a reaction. Scientists are doing studies to find out whether people with celiac disease can tolerate oats. Until the studies are complete, people with celiac disease should follow their physician or dietitian’s advice about eating oats.
Plain meat, fish, rice, fruits, and vegetables do not contain gluten, so people with celiac disease can eat as much of these foods as they like. Examples of foods that are safe to eat and those that are not are provided below.
The gluten-free diet is complicated. It requires a completely new approach to eating that affects a person’s entire life. People with celiac disease have to be extremely careful about what they buy for lunch at school or work, eat at cocktail parties, or grab from the refrigerator for a midnight snack. Eating out can be a challenge as the person with celiac disease learns to scrutinize the menu for foods with gluten and question the waiter or chef about possible hidden sources of gluten. Hidden sources of gluten include additives, preservatives, and stabilizers found in processed food, medicines, and mouthwash. If ingredients are not itemized, you may want to check with the manufacturer of the product. With practice, screening for gluten becomes second nature.
A dietitian, a health care professional who specializes in food and nutrition, can help people learn about their new diet. Also, support groups are particularly helpful for newly diagnosed people and their families as they learn to adjust to a new way of life.
Damage to the small intestine and the resulting problems with nutrient absorption put a person with celiac disease at risk for several diseases and health problems:
Celiac disease is the most common genetic disease in Europe. In Italy about 1 in 250 people and in Ireland about 1 in 300 people have celiac disease. It is rarely diagnosed in African, Chinese, and Japanese people.
An estimated 1 in 4,700 Americans have been diagnosed with celiac disease. Some researchers question how celiac disease could be so uncommon in the United States since it is hereditary and many Americans descend from European ethnic groups in whom the disease is common. A recent study in which random blood samples from the Red Cross were tested for celiac disease suggests that as many as 1 in every 250 Americans may have it. Celiac disease could be under diagnosed in the United States for a number of reasons:
More research is needed to find out the true prevalence of celiac disease among Americans.
People with celiac disease tend to have other autoimmune diseases as well, including
The connection between celiac and these diseases may be genetic.
Dermatitis herpetiformis (DH) is a severe itchy, blistering skin disease caused by gluten intolerance. DH is related to celiac disease since both are autoimmune disorders caused by gluten intolerance, but they are separate diseases. The rash usually occurs on the elbows, knees, and buttocks. Although people with DH do not usually have digestive symptoms, they often have the same intestinal damage as people with celiac disease. DH is diagnosed by a skin biopsy, which involves removing a tiny piece of skin near the rash and testing it for the IgA antibody. DH is treated with a gluten-free diet and medication to control the rash, such as dapsone or sulfapyridine. Drug treatment may last several years.
Check Out Our Reviews & Testimonials
At Midwest GI Health we are proud to share our patient referrals from Healthgrades, Vitals, Google and Facebook. Please take some time to see how pleased our patients are with our professionalism and quality of care.
After years and years of stomach issues and having the same simple tests done with no results, I saw Dr. Taormina and he’s actually trying to help figure it all out, new tests…

The staff was very professional and friendly. The exam was explained by a nurse and the Anesthesiologist then came in to explain what she was going to do. Dr Taormina came…

The facility is small enough you don’t feel like a number and big enough you know they have what they need in case of an emergency. Dr Taormina is easy to talk to and answers all questions. Explains everything well, easy to understand. The group of nurses are also great!

Free Resources